At Alterdoctor, we are fascinated by individuals who further the boundaries of care. We are equally fascinated by how professionals expand their own milieu interna. Once in a while we come across doctors who do both seamlessly. Today we will explore aspects of empathy with Dr Mark Lewis, an oncologist and a gifted writer who often shines a light on that very important attribute through his writings.
Dr.Mark Lewis ,a Medical Oncologist is director of gastrointestinal oncology at Intermountain Healthcare in Salt Lake City, Utah .He diagnosed his own hereditary cancer syndrome during the beginning of his oncology residency and underwent a Whipple’s surgery for Pancreatic Neuroendocrine tumour. His article on patient encounters post surgery can be found here: http://alterdoctor.in/how-i-envy-you-fridays-with-paul/
AD:Thank you, Dr Lewis, for talking with us at Alterdoctor. You are an oncologist and a writer with a very active social media presence through your blogs, twitter and more. Does your writing predate your medical career or did it start as a vehicle to express your thoughts as a professional?

ML:I started diarizing my career during my oncology fellowship. First and foremost, the start of my training coincided with my self-diagnosis with a rare hereditary tumour syndrome and I realized it would be valuable to record my experience as a patient, partly as a chronicle for my son to whom I have in turn transmitted the mutation. Secondly, I came to recognize the enormously cathartic nature of trying to sublimate the complicated feelings of an oncologist into words, perhaps first captured in my essay “A Balancing Act”: https://ascopubs.org/doi/full/10.1200/jco.2011.41.5695
AD:Knowledge of the Classics especially Greek really enriches your ability to express. How important do you feel it has been in shaping you as an individual- My a writer and more?

ML: When my essay “Between Scylla and Charybdis” was published in the New England Journal of Medicine my wife – who is so much more practical and wise than I am! – asked me why I didn’t call it “Between A Rock and a Hard Place,” which would have idiomatically captured the same tension. But I think story telling is such a resonant form of communication and clearly the enduring nature of Homer and our classicists speaks to the timeless chord they strike. On a personal note, my father was a great lover of myth, writing:
“A notoriously multiform and slippery notion, resistant to easy definition, myth has sometimes stood, if not bluntly for the false, at least for an indirect, unfactual, and generally obsolescent expression … [But] myth is the imaginative use of symbol and parable, of the poetic and pictorial, to express the inexpressible. Far from false, it is the only way to come close to what is ultimately true.” – Alan E. Lewis, Between Cross and Resurrection
AD: You often mention the spiritual dimension and particularly your family when discussing aspects of empathy. Important as that has been to you, how do you see a similar rootedness shaping empathy in individuals?
ML: I have been quite candid that I would likely have entered the ministry if not for a crisis of faith during my adolescence. Perhaps as a means of self-assurance, I have since come to see medicine – and oncology in particular – as analogous to pastoral care delivered within the bounds of our secular discipline. One need not have a religious faith to practice good medicine, but, as Dr. Francis W. Peabody reminded us, “the secret to caring for the patient is caring for the patient”. Buried in that seeming tautology is the core interaction in medicine between a healer who sees a person in need of healing.
AD: Was it a conscious decision to take up Oncology given the personal tryst with Cancer ?
ML: Yes, I almost felt a filial responsibility to enter oncology after losing my Dad. When I got to medical school and learned that, short of psychiatry, it’s considered the specialty where you have the closet longitudinal relationships with patients, I felt validated in my decision, as I feel like I get to provide a version of my father’s pastoral care in the secular space.
AD: A running joke is often that you would find the most amount of hypochondriacs within the medical student community. But yet, it was during your residency that you diagnosed yourself with MEN1 syndrome. Can you please tell us the cascade of events that led to this?
It was, in some ways, very poor timing to be self-diagnosing at the beginning of cancer training, when complaints of a hereditary tumor syndrome naturally included hypochondriasis in the differential diagnosis! The eureka moment came when, in the process of investigating abdominal pain, I was found to be hypercalcemic.
ML: My father had the same metabolic disturbance for his entire adulthood, and I remembered from medical school that there were very few conditions that would lead to consecutive generations with hypercalcemia. Once familial hypocalciuric hypercalcemia was ruled out, it was essentially MEN1 by process of elimination. ( Captured in detail this essay for Journal of clinical oncology https://ascopubs.org/doi/pdf/10.1200/JCO.2011.35.1122 )
AD: Being a person with Multiple Endocrine Neoplasia, now post major surgery, gives you a hard-earned perspective to what it means to be in your patients’ shoes. You have written about ‘how you started your career in the hopes of providing sympathy and providentially discovered a wellspring of empathy’- has that fundamentally changed you in patient care?
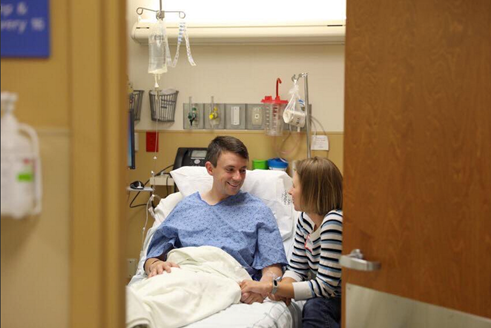
Morning of Whipples, with wife, Dr. Stasha Lewis, at bedside: 
Date of first discharge –He would be readmitted 36 hours later with delayed gastric emptying: 
This was when NG tube was finally removed, 5 weeks post-op, a truly joyous occasion!
ML: I still have not had the “taste of my own medicine” insofar as the chemotherapy I prescribe. But I do understand the risk/benefit calculus that a patient goes through when faced with a life-threatening diagnosis that can only be remedied by invasive and/or toxic means. Brené Brown defines empathy as “the incredibly healing message that you are not alone.” No matter how much of their earthly time remains, and whether the goal of care is cure, control, or comfort, we can tell our patients with absolute certainty that we will not abandon them to the unknown.
AD:During your years of clinical encounters with patients, at any point of time, were you beseiged with thoughts of fear, pessimism and your mental framework when counselling oncology patients
ML: I think most oncologists are optimists by nature, not pessimists. I have actually found my own patients to be an enormous source of inspiration in how they handle the shifting sands of their disease. And I tell them there is always hope, whether for cure, control, or comfort; hope is never extinguished, and it can span from durable remission to a dignified death.
AD:Being an empathetic professional, we guess, also comes with the ability to understand the view points of your detractors. There are a few examples that you quote, both towards the medical community (#doctorsaredickheads) and personal (the twitter heckling). Where do you draw the line in engaging them?
ML: One of my wisest friends, an entrepreneur and technological maven, reminded me that the greatest currency is not money, but time. I used to be naïve enough to think that I could sway an argument with solid logic and by citing substantiating examples. I have since come to realize that some people online only want to occupy your attention so that you can’t actually devote energies to the channels and causes that matter to you. The block button on Twitter tends out to be a marvellous device if you find a partner in conversation is diverting your attention more than necessary! Dr. Don Dizon (@drdondizon) also has these sage words: never Tweet exhausted, inebriated, or angry!
AD: Sub specialty healthcare, for example hematology-oncology, is often practised as a highly algorithmic field. You have made the insightful comment of ‘yet to meet a patient who cares more about time to progression than quality of life’. Can the twain meet?
ML: I am seeing an increasing rejection of surrogate endpoints that matter little to patients. At the 2019 ASCO annual meeting, Dr. Vinay Prasad astutely observed the two undeniably meaningful outcomes in oncology are longevity and quality of life, with almost literally every other metric being less important, at least to those under our care and their advocates. Yes, the twain can meet if we discard sophistry like “manageable toxicity” and embed patient-reported outcomes in trial design, ideally soliciting key stakeholder input at the level of protocol development.
AD: A natural progression through empathy, one would presume, is advocacy. What are your views on patient advocacy?
ML: The self-advocating patient is becoming the most powerful force in healthcare. And, with the notable exceptions of paywalled articles and closed conferences, the informational playing field is becoming more level for all of those who engage in healthcare, whether as practitioners or recipients. The model of paternalism has been toppled like a statue in a coup d’état and we can now do more than pay lip service to the notion of shared decision-making.
AD: Nature and nurture shapes us as individuals. While we discuss empathy, it’s quite easy to see how both have played a role in your case. Can we can inculcate empathy in Medical professionals and do you have any suggestions? (Besides reading your blog and following you on twitter 😊)
ML: Siddhartha Mukherjee, writing in The Gene, beautifully explicates what happens to us as the sum of heredity + triggers + environment + chance. The last might just as well be described as Shakespeare’s slings and arrows of outrageous fortune, and it should remind us all that, when looking at the patient before us, “there but by the grace of God go I”.
Siddhartha Mukherjee, writing in The Gene, beautifully explicates what happens to us as the sum of heredity + triggers + environment + chance. The last might just as well be described as Shakespeare’s slings and arrows of outrageous fortune, and it should remind us all that, when looking at the patient before us, “there but by the grace of God go I”.
AD: Finally, what would your message be to the oncology community (doctors, caregivers, patients) …..
Not all of us can have complete empathy with patients if we have not experienced the same conditions as them but we can certainly have sympathy for all!